So what is Diabetes?? There are different types, it’s important to know the differences. The 3 main types are as follows:
Type 1 (formerly known as Juvenile Diabetes). If you have type 1 diabetes, your pancreas does not make a hormone called insulin. When we eat, our body breaks down the food into energy for our muscles, organs, etc. Insulin is the key that converts the food into useful fuel (glucose) that then gets taken up by our cells. Without insulin, this cannot take place and therefore the fuel/glucose gets built up in the bloodstream instead of getting into our cells. This can cause some nasty problems. Because type 1’s make zero insulin, they have to replace it with man-made insulin, by injections or via an insulin pump. There is no cure. Type 1’s are on insulin for life. Unless they receive a pancreas transplant, or transplant of the cells that make insulin. There is no proven cause of type 1. It is not caused by eating too much sugar. One leading theory is that it is an auto-immune disorder and quite possibly hereditary. Only 5% of people with diabetes are type 1.
Type 2. The more popular type. It accounts for about 95% of all diabetes cases. If you have type 2, your pancreas still makes insulin but you have what’s called insulin resistance. Your body isn’t able to properly use the insulin being made. Type 2’s may be treated in a variety of ways. Some people can manage with lifestyle changes (diet, exercise, weight loss), some need oral medications, others may need insulin to manage. There is a strong family history/genetic link with type 2. Lifestyle also plays a factor.
Gestational. This basically means you have diabetes while you’re pregnant, usually the onset is about halfway through pregnancy. You didn’t have it prior to getting pregnant and you most likely won’t have it after baby is born (although your risk is higher for developing type 2). It’s a little like type 2. Somehow the mom’s body becomes more resistant to insulin and requires changes to diet, and possibly the addition of meds, including insulin during the remainder of the pregnancy.
With all types of diabetes, the blood sugar must be checked routinely. As a type 1, I check it at least 8 times a day with this handy dandy machine. More than that when I’m pregnant.
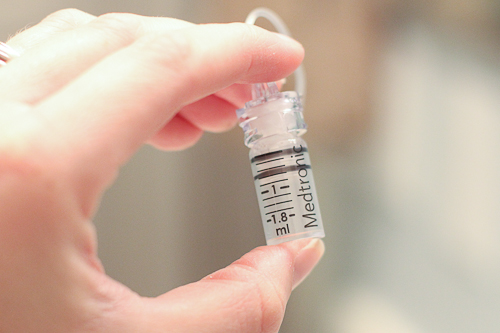
I treat my diabetes with an insulin pump. I use a medtronic paradigm 523 pump. And yes it’s pink! I love it. LOVE it. Every 3 days I have to fill up a special syringe with insulin and place it into the pump. The syringe is hooked up to a very thin flexible tubing that connects to a plastic catheter that gets inserted into my body via a needle.
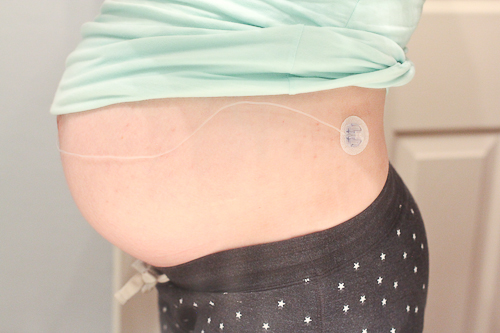
I change that insertion site usually every 3 days as well. I can place it on my abdomen, love-handles, lower back, even my upper arms and thighs (which I almost never do).
Then before I eat, I check my sugar. I tell the pump what my sugar level is and how many carbs I’ll be eating. The pump is pre-programmed by my Dr and pump trainer with a very specific, individualized formula that calculates how much insulin I should take based on the numbers I punched into it. I can then tell it to give me that amount or I can adjust it. I do this for every meal/snack. I also check my sugar 1-2 hours after eating and if my sugar is higher than recommended I can then use the pump to adjust my sugar levels.
Its a constant balance. Lots of trial and error as there are several things, not just food, that can affect blood sugar levels. My pump isn’t water tight so I have to disconnect it when I shower, go swimming etc. The plastic “needle” stays in place in my body so I don’t have to replace the whole thing, just the pump portion. When its all hooked up, I personally like to keep my pump hooked on my bra, out of the way!
When I’m not pregnant, I see my endocrinologist every 3-4 months to show him my blood sugar logs and check blood work. During pregnancy I’ve been seeing him every month to stay on top of my sugars, my pump settings, my a1c and my thyroid levels. An A1c is a blood test that is basically an average of blood sugar over the past 2-3 months. It is often used as an indicator of how well (or not) diabetes is being “managed.”
Based on the ADA, here are the recommended blood sugar levels and A1c’s for “most adults with diabetes.” As well as those levels for pregnancy.
Not Pregnant
A1c: less than 7%
Before meals: 70-130
1-2 hours after meals: less than 180
Pregnant
A1c: less than 6%
Before meals and at bedtime/overnight: 60-99
1-2 hours after meals: 100-129
Every body is different, every person copes in different ways and adjusts to insulin in different ways. I’ve had endos (Endocrinologists) that nit-pick every high number and focus on that. My current endo cares mainly about the lows. Diabetes isn’t treated with one specific formula, each person requires an individualized plan of care.


This blog is wonderful and really has given me some insight into the world of a person who has diabetes, esp one who is pregnant. I am amazed at what you all go through on a daily basis. I love your openness and the sprinkles of humor throughout. Humor is such a gift! Keep writing please!